Q:What is the mode of transmission for covid-19?
Ans:Sars-CoV-2 virus is transmitted directly through droplets or aerosols generated when a covid-19 patient coughs or sneezes.
Q:What is the incubation period?
Ans:Incubation period is the time interval between the entry of organism into your body and appearance of first symptom, this is 2 to 14 days for covid-19. (Mean: 5 – 7 days)
Q:Who are said to be “At risk ” population?
Ans:People with hypertension, diabetes mellitus, cardiac illness, immunosuppressed individuals, people on immunosuppressant (post organ transplant), children with congenital cardiac problems, asthma and healthy individuals exposed to covid-19 positive cases are prone to get severe disease from Sars-cov-2 infection, hence considered to be population at risk.
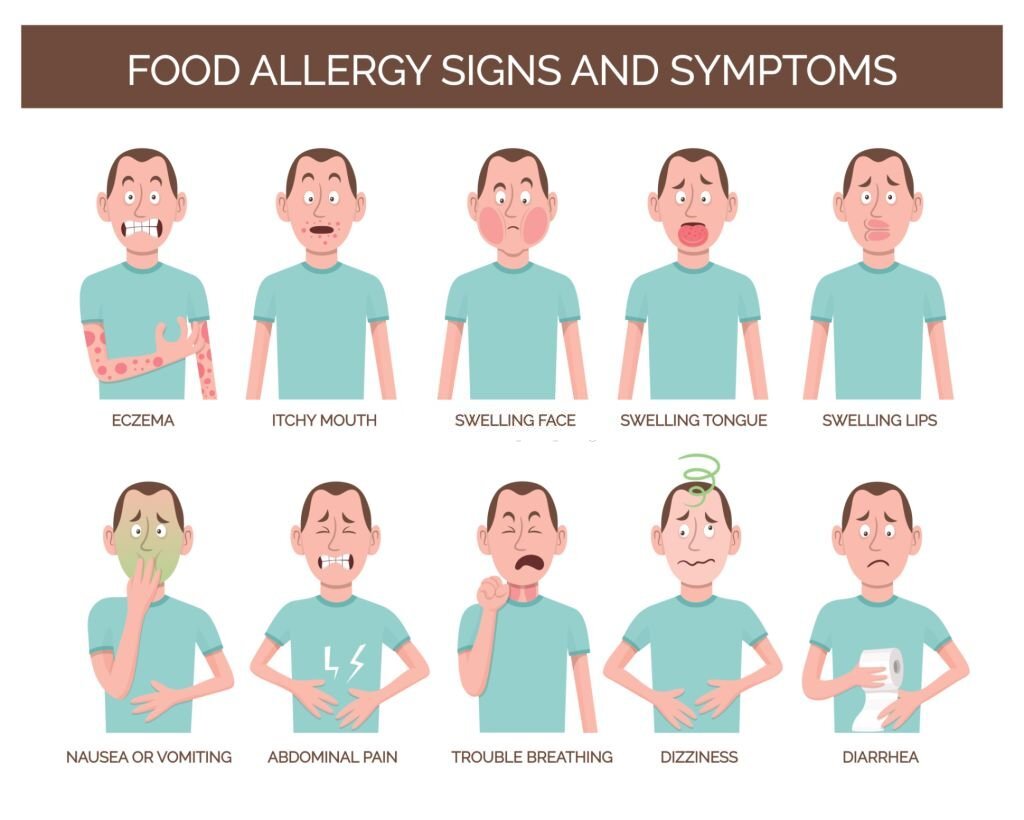
Q:What are the common symptoms of covid-19?
Ans:Symptoms are the apparent features experienced by the patient in an illness. More common symptoms in covid-19 disease are fever, sore throat, dry cough, fatigue, body ache, headache, diarrhoea, loss of taste, loss of smell and breathlessness.
Q:Is there any test that can be done at home to diagnose covid-19?
Ans:Yes, there are commercially available kits. It is called as rapid antigen test and the results are obtained in 15 min while still being at the comfort of your home.
Q:Which is the best test for covid-19?
Ans:Real Time – Reverse Transcription Polymerase Chain Reaction, commonly called as RT-PCR test or the swab test widely used to detect SARS-CoV-2 virus and currently being considered best for covid-19 patients.
Q:What is the confirmatory test for covid-19?
Ans:RT-PCR is the gold standard frontline test for novel coronavirus. It detects the virus from samples of throat or nasal swab of people with symptoms or high-risk individual who might have come in contact with covid-19 positive patients.
Q:What is the right time to do RT-PCR?
Ans:A false negative covid-19 test results can be due to testing too early or too late. The ideal time for testing by RT-PCR should be after 48 hours of onset of symptoms. (2nd or 3rd day)
Q:Should RT-PCR be done for one day fever with minor respiratory symptoms?
Ans:Yes, given the current situation of a pandemic it is advisable to confirm the nature of illness, thus aiding better treatment and prevention of spread of infection.
Q:What is the right to do CT scan?
Ans:CT scan to be done only on the advice of a doctor. CT chest is indicated only in patients with breathlessness, SPO2 <94% in room air and in severe disease with worsening respiratory status or breathing difficulty.
Q:What must be monitored after being tested positive for covid-19?
Ans:Along with timely intake of medicines prescribed by treating physician, patient in home quarantine must monitor SPO2, temperature, urine output and watch for symptoms like easy fatigability or breathlessness.
Q:How often should we check SpO2 during home quarantine?
Ans:SpO2 should be checked in every 4-6 hrs once.
Q:What is the normal SPO2 level?
Ans:SPO2 refers to the oxygen saturation level in our body. It can be monitored at home with the help of a pulse-oximeter. SPO2 > 94% in room air is considered to be normal.
Q:What is the approach based on saturation level?
Ans:If SPO2>94% in room air in patients with symptoms of covid-19 and RT-PCR positive result, home quarantine is advised with prescribed medication. SPO2<94% in room air or >94% in room air with 5% drop after a 6-minute walk test calls for hospitalization.
Q:What is a 6-minute walk test?
Ans:This is a simple and effective test to measure healthy functioning of heart and lung suggested in covid-19 patients with mild symptoms. The patient in home quarantine with SPO2>94% in room air is made to walk in the confinement of their room 6 min non-stop without oxygen support. Drop in SPO2 level of 5%, light headedness or breathlessness indicates these patients need prompt medical assistance with oxygen support.
Q:What are the signs of breathing difficulty in covid-19?
Ans:Fast breathing, breathlessness can be signs of respiratory distress. Respiratory Rate (RR) is number of breaths a person takes in a minute.
- Normal RR: 16 to 18 breath / Min (in asymptomatic patients)
- Mild disease – RR: <24 breath /Min (SPO2 > 94% in room air)
- Moderate disease – RR: 24 – 30 / Min (SPO2 90% to 94% in room air)
- Severe disease – RR: > 30 /Min (SPO2 < 90% in room air)
Q:What is the period of quarantine?
Ans:Covid-19 patients are kept in isolation for 14 days to prevent spread of infection to healthy individuals.
Q:Which is considered day1 of illness? Day of onset of symptom or reporting positive with RT-PCR?
Ans:For treating, planning of investigations, and deciding on treatment strategies Day1 of illness is a very important criteria and is always counted from the day of onset of first symptom.
Q:What is the period of quarantine for a healthy individual exposed to covid-19 patient?
Ans:Irrespective of onset of symptoms susceptible people are quarantined for 14 days after being exposed to covid-19 patients.
Q:What are the measures to be taken during home quarantine with asymptomatic senior citizen sharing a home with covid-19 patient?
Ans:It is recommended that covid-19 positive individual in home quarantine use separate rooms with attached bathrooms, use separate utensils, avoid direct contact with elderly people.
Q:Is there any food restriction for covid-19 patients?
Ans:No food restrictions for patients suffering from covid-19. Plenty of oral fluids and protein rich diet is recommended for speedy recovery.
Q:Can I share medicines of covid-19 infected family member when I have symptoms of covid-19?
Ans:No. Medicines should be taken only after consulting a physician.
Q:Can I continue my regular medicines as prescribed earlier?
Ans:Yes, all regular medicines taken for comorbid conditions should be continued as advised, for clarification of doubts regarding the same contact family physician. Changing doses without proper prescription is strictly not recommended.
Q:What are the warning signs to consult a doctor immediately?
Ans:Patients in home quarantine need to be watchful for warning signs which may be an indication for a need to escalate the treatment. Common warning signs are persistent high-grade fever, shortness of breath or breathlessness, SPO2<94% in room air, easy fatigability, persistent vomiting, excessive drowsiness, fits.
Q:What are the advice for breastfeeding in covid-19 positive mother?
Ans:The baby is to be isolated from mother. Expressed breast milk is fed to baby with paaladai or spoon by non-covid family member following good hygienic practices.
Q:What are the procedures to be followed when isolation of baby is not possible?
Ans:In a nuclear family where both parents are covid-19 positive, mother can wear a mask, sanitize hands properly and feed the baby expressed breast milk with paaladai or spoon. The cradle can be kept at a distance of 6 feet from mother’s bed in same room. The room should be well ventilated.
Q:What are the procedures to be followed if baby is also symptomatic?
Ans:The child should be taken to consult a paediatrician immediately.
Q:Can a mother with covid-19 infection breast feed?
Ans:Although the ideal way is to give expressed breast milk, in unavoidable situation infected mother can breast feed after proper sanitizing and wearing a face mask.
Q:Can a mother with fever during covid-19 infection breast feed?
Ans:Yes, yet again, giving expressed breast milk with paaladai or spoon is the better method.
Q:How long can cough be present after covid-19 infection?
Ans:Occasional cough for 2 weeks is taken to be normal when saturation levels are more than 94% in room air. Consult a doctor if cough persists along with breathlessness and drop in SPO2.
Q:What are the procedures to be followed while using oxygen concentrator during post covid phase at home?
Ans:An oxygen concentrator is a medical device that works by concentrating oxygen from the ambient air and aiding the patient in breathing easily at home. While using, SPO2 levels should be checked every 4-hour, water in humidifier is to be changed every day. Any drop in SPO2 level or shortness of breath should be addressed immediately by consulting a doctor.
Q:What are the measures to be taken for chest tightness or excessive tiredness at home post covid?
Ans:Patients are advised to continue medicines a prescribed during discharge by treating physician, monitor saturation levels (spo2), continue breathing exercises and use spirometer to improve lung capacity. Report to hospital immediately if chest tightness, excessive tiredness and breathlessness develops.
Q:Should we wear a mask post recovery while going outside?
Ans:Yes, even after a period of 14 days it is always advisable to wear mask, avoid touching face, and maintain social distancing while going outside. Remember, it is best to avoid stepping out of home unnecessarily.
Q:After 14 days of isolation, can the room used by patient who tested positive for covid-19, be used by a healthy individual immediately?
Ans:The room should be cleaned thoroughly twice before being used. One normal cleaning with soap and water followed by one deep cleaning with disinfectant is recommended. Air conditioner vent and filter should be cleaned, and air dried under sun, furniture should be wiped with 70% alcohol solution, fabrics can be soaked in Dettol for 30 minutes and washed with detergent. The room can be opened for routine use after a gap of maximum 12 hours after cleaning.
Q:Can things such as linen and utensils used by covid-19 patient be reused by other family members?
Ans:Yes, after following strict disinfection procedures (washing the utensils with detergent, hot water and drying in sunlight) things can be reused.
Q:Is there any test to be done prior to covid-19 vaccination?
Ans:No testing needs to be done prior to vaccination.
Q:Covid-19 patients received convalescent plasma/ monoclonal antibodies, when should they take vaccine for covid-19?
Ans:Three months from date of discharge from hospital.
Q:Coronary artery disease patient on blood thinners, when should I stop medicines prior to vaccination?
Ans:Blood thinners and other cardiac medications prescribed by cardiologist should be continued regularly without fail until mentioned otherwise by treating doctor as blood thinners are NOT contraindicated for covid-19 vaccination.
Q:If a person is infected with covid-19 after receiving the first dose of vaccine against covid-19, when should he/she be given the second dose?
Ans:Vaccine can be administered 3 months after recovery from illness as second dose. There is no need to restart the schedule.
Q:What is the right age for vaccination?
Ans:All individuals above 18 years of age are eligible to receive covid-19 vaccination.
Q:Is there any vaccine available for children below 18 years against SARS- CoV- 2?
Ans:No, although available in other countries, currently there are no approved vaccination in India for children below 18 years of age against covid-19.
Q:What is the ideal time for vaccination in patients with any major disease or needing ICU care?
Ans:Any illness can cause immunosuppression in an individual and thus vaccine should be administered 4-8 weeks after recovery.
Q:What is the ideal time to get vaccinated after recovering from covid-19 infection?
Ans:During a covid-19 infection, antibodies are produced by our body against novel corona virus, but there will be a decline in antibody levels and the vaccine will help to boost up immune response. Thus, vaccination is recommended after 3 months of recovery from illness.
Q:Can a nursing mother take vaccination against covid-19?
Ans:Yes, surely. Government of India, department of health and family welfare had recommended all lactating women to be vaccinated against covid-19.
Q:Can a pregnant woman take vaccination against covid-19?
Ans:No, as per current updated guidelines, pregnant women are advised not to take the vaccine.
Q:Can a mother who has taken vaccine for covid-19 breast feed?
Ans:Yes, vaccine is not a contraindication for breast feeding and all nursing mothers can continue to breast feed after taking vaccination.
Q:If child has suffered from covid-19 when can we resume normal vaccination?
Ans:Child can be scheduled for regular vaccination 4 weeks after recovery from covid-19.
Q:When can a child exposed to covid-19 positive parents, but due for normal vaccination be vaccinated?
Ans:Ideally a 3-week observation period is recommended. If child remains asymptomatic after this period, child can be started on regular vaccinations.
Q:What is the ideal time for blood donation after vaccination?
Ans:Healthy individual who has received vaccine against covid-19 can donate blood after 14 days from date of vaccination.
Q:What is the ideal time for blood donation after a negative RT-PCR result?
Ans:Ideal waiting period prior to donating blood is 14 days/ 2 weeks.
Q:When should I repeat RT-PCR test after being infected with covid (proven cases with positive RT-PCR)?
Ans:A repeat test of RT-PCR to prove negative covid status is not necessary. Please do not repeat RT-PCR test for covid-19 without recommendation from a doctor.
Reviewed By:
DR.ABINAYA P V
CONSULTANT – GENERAL MEDICINE
MBBS, MD GENERAL MEDICINE